Healthcare reform in HK
13 June 2008
What do you think? Take our Healthcare poll
On 13-Mar-08, the HK Government published a consultation document on healthcare reform, titled "Your Health Your Life". This is a combination of reforms to the healthcare system, such as a territory-wide electronic health record system, and proposals to change the financing system.
Rather unwisely, the government has linked the two together, saying that it can't implement service reforms without changing the financing system. They might have titled the paper "Your Wealth or Your Life". In reality there is no connection between the two, and the linkage carries the implied threat of inaction unless the community agrees to mandatory savings or insurance. Yet surely if an electronic records system or a register of family doctors, or other service reforms are worth implementing, then they should already be underway.
The structural surplus
It is not as if the Government is short of money - it stashes most of its savings in the Exchange Fund, which, along with the accumulated surplus, amounted to about HK$1,104bn at 30-Apr-08. That excludes the $359bn in the currency board account which backs the US$/HK$ peg. By comparison, on 31-Dec-98, the savings amounted to HK$667bn. So the Government has salted away an additional $437bn in just over 9 years, not to mention the billions stashed away in liquid investments elsewhere, such as the $5bn hoard in the MPF Authority, the $4bn in the SFC, the $8bn in the Urban Renewal Authority, or the $53bn in the Housing Authority. Whoops, we mentioned it.
If you search the Government press releases for the phrase "structural deficit", you will find the last mention of it over 3 years ago, in then Financial Secretary Henry Tang's budget wrap-up speech on 27-Apr-05, when they were still trying to persuade the public to swallow a Goods and Services Tax in this constitutional free port. That talk has been abandoned, and when you look at long-run data it is obvious that we have a government which hoards public money by running a structural surplus, and then runs a quasi-Sovereign Wealth Fund in the form of the Hong Kong Monetary Authority's Exchange Fund, which invests in bonds and equities (including HK equities) rather than returning wealth to the people as most democracies do.
Measuring expenditure
The total public-sector expenditure on health in 2007-08 for our population of about 7 million was about HK$33.5bn and will rise to $35.8bn in 2008-09, or about $5,100 per person, according to figures published with the latest budget (see page 9). These are General Revenue Account (GRA) figures. In the consultation paper, they use a more broadly-defined "Domestic Health Accounts" (DHA) figure, based on OECD standards, which throws in additional cost allocation from non-health departments such as pest control by the Food and Environmental Hygiene Department, or building design from the Architectural Services Department. Unfortunately, these DHA numbers are not normally calculated by the Government - they had to commission a study just to find out what they are. On average, for the five years from 2000/1 to 2004/5, DHA was about 15.4% higher than GRA.
Crude threats
With our structural surplus and humungous reserves, we can well afford to spend more to improve the health care system and shorten waiting lists, with or without financing reform. Our doctors are overworked - there is now talk of cutting their hours to "just" 65 hours per week, and limiting on-call shifts to 24 hours - they are true heroes, but do you really want your life in the hands of someone who might not have slept since yesterday?
In the paper, the Government trots out a series of crude threats, such as ever-increasing waiting times for surgery. However, whether waiting times increase or decrease is entirely within the Government's control - by hiring and training more healthcare professionals, and expanding facilities, waiting lists can easily be cut. The queuing system is a form of rationing, because those who prefer not to wait and can afford private care will pay for private treatment. The longer the queue, the greater the number of people who will go private, while for those who cannot afford private treatment, some will simply die from the condition for which they are waiting treatment or from something else while waiting, thereby reducing the number of treatments given.
Unreliable projections
One thing we know for sure about 25-year projections by governments or anyone is that they are almost always wrong by a wide margin from the final outcome. The HK Government has consistently over-estimated population growth in the past. Now it claims that public health expenditure will grow at 5.7% per year from 2004 to 2033, compared with 3.4% per year for real gross domestic product (GDP), our economic output. This would raise public health costs from 2.9% of GDP in 2004 to 5.5% of GDP in 2033, 25 years from now, while total healthcare (including private expenditure) would grow at 5.4% p.a. from 5.3% to 9.2% of GDP.
If this trend were to keep up indefinitely, then 100 years from now, we would be spending 38.7% of GDP on total healthcare, and by the year 2158 the figure would be 100% of GDP, an economic impossibility, since it would imply everyone was working in healthcare and nobody was doing anything else to pay for it. Clearly, at some point, the growth of health costs relative to the rest of the economy has to flatten out. The truth is that nobody knows what the figures will look like 25 years from now. Throughout history, technology has a track record of lowering costs in most areas of the economy - for example, the cost of publishing this article online is trivial. But in medicine, conventional wisdom internationally is that technology will increase costs indefinitely, extrapolating from the trend over the last 20 years. That is clearly impossible. The past is not a reliable guide to the future.
Advances in medical research are changing the landscape, and some of them will undoubtedly cut costs. 40 years ago, when people now in their 60s were first getting hooked on nicotine, it was not well accepted that smoking cigarettes can cause cancer and heart disease. Now it is, and the smoking population has declined dramatically, which should lead to lower total expenditure on treating those diseases. Some 90% of lung cancer patients are smokers. Early screening for other cancers, such as pap smears for cervical cancer and the HPV vaccination, will also cut the death rate and improve economic output - live people are more productive than dead people. Advances in genetics in future will allow for preventative screening of those most at risk of various diseases based on their genes. Today only a handful of people in the World have had their genome sequenced, but in 2033 this will probably be common and even done at birth.
We've been here before
Back in 1993, the Government issued a report titled "Towards Better Health" and known as the Rainbow Report, which Webb-site.com is putting online for the first time. It warned of escalating health care costs. Public spending on healthcare was then 2.3% of GDP in fiscal 1992/3. Later, on 12-Apr-99, the Government published a consultation paper known as the Harvard Report, "Improving Hong Kong's Health Care System: Why and For Whom?". Just 9 years later, the Harvard Report projections are widely out of line with reality.
Webb-site.com has looked at the actual outcome. The current consultation paper gives us DHA expenditure figures for 2000/1 up to 2004/5. For the other years, we have then taken the actual Total Public Expenditure on health reported in budgets from 1996/7 up to 2007/8, and the budget estimate for 2008/9, and added 15% to estimate the DHA figures. For GDP, we have actual figures up to 2007 and a projected figure for 2008. Then, we've compared the outcome with the Harvard projections of 1996-2016, and the projections in the latest consultation paper, from 2005 to 2033. And here's the result:
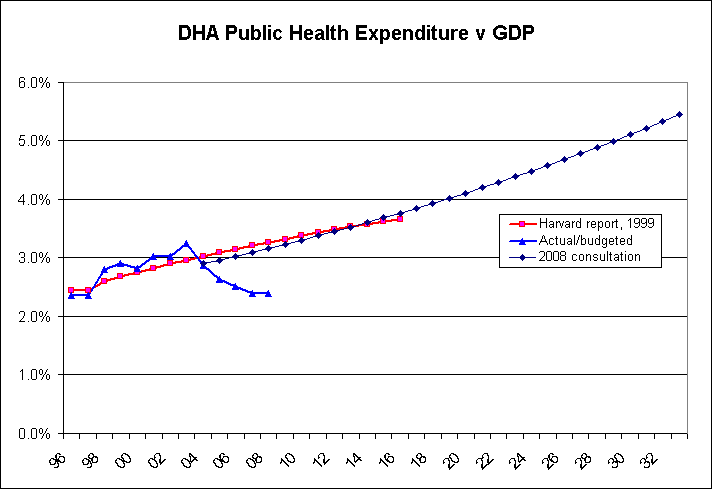
As you can see, after climbing during the economic slowdown after the 1997/8 Asian financial crisis, and again during SARS in 2003, the actual public health expenditure as a share of GDP is now back down to just 2.4%, where it was in 1997 and just 0.1% higher than 1992/3 (the Rainbow Report), 16 years ago. But if you believed the scary Harvard estimates 9 years ago, then by now we should be spending 3.3% of GDP, or about 38% more than we actually are spending in 2008/9, as a share of GDP. If that is how reliable the projections are after 9 years, then they are almost completely random after 25 years.
This year's consultation comes with another set of projections shown in the graph above. You will notice, incidentally, that in all of these "new" consultation papers, the historic figures stop in 2004/5, suggesting that they were prepared before the 2005/6 figures were available and have been on the shelf since then, waiting for a political window of opportunity to launch the consultation.
Starting with 2.9% of GDP in 2004 and projecting forward, the current consultation projects public DHA health spending to be 5.2% of GDP in 2033. Even by 2010/11, they expect us to be at 3.3%, whereas we now know with some certainty that it will be about 2.4% in 2008/9. Those projections were out of date before they were published, and the Government should have admitted that.
To be clear, we are not predicting that public healthcare costs as a share of GDP will remain at 2.4% forever. Real healthcare expenditure will certainly go up, if only because of the ageing population, and GDP may, or may not, go up faster than health expenditure, as it has since 2004. As GDP is much harder to project, so are health costs as a share of GDP, and that is what matters for fiscal planning purposes. All we are demonstrating in the above analysis is that you have about as much chance of accurately projecting this figure as you do of accurately predicting the Hang Seng Index 25 years from now.
Demographic projections are shaky too
Even the "ageing population" story stands on shaky ground. We know that the existing population will age, but we don't know how many people will move here or leave. Recently, we have been inundated with mainland mothers happily paying $39,000 per pop to give birth in a public hospital in Hong Kong and claim right of abode for their baby under the Basic Law. This is a good thing. Many of those children (whose parents are affluent by mainland standards) may eventually return here for education and to work, reducing the demographic ageing and strengthening the economy. In the opposite direction, schemes may be devised to incentivise retirees to move to the mainland where the cost of living is lower, and to build Hong Kong-managed hospitals there where land and staff will be cheaper.
Further, the workforce may be replenished by inward migration. Currently HK has various barriers to discourage this, and then devises schemes for the "right" kind of immigrants, such as the Quality Migrant Admission Scheme and the Capital Investment Entrant Scheme. But as the domestic workforce shrinks, those barriers can come down without political objection, and we can welcome immigrants to replenish the workforce, contributing to the economy and helping support the welfare and healthcare system. With the economic recovery in recent years, the Government has already begun to lower the barriers, for example, allowing foreign students to remain here to seek work after graduation.
Pre-emptive screening
Another area where more creative thought is needed is in preventative care. Future public expenditure could be avoided if age groups at risk of common diseases such as diabetes are screened and counselled on their lifestyle choices. Early detection could reduce treatment costs and return workers to the economy, while counselling those with unhealthy habits would motivate change when they learn how much it would cost them in terms of reduced life expectancy, reduced income and increased medical expenses if they don't look after themselves.
An economic evaluation should be made of the costs and benefits of screening. For rare diseases, screening the entire population would not be cost effective, but for common diseases, it probably would. On the spectrum of incentives, we shouldn't necessarily stop at subsidised or free screening. It may actually save money in the long run if we offer to pay people to be screened, thereby increasing the number of people who come in, particularly among the lower income groups where the payment would mean more. These are the same people who will be unable to pay for healthcare when they need it, resulting in greater public expenditure. There is also a correlation between education and income (particularly among the elderly), so the lower-income groups are in greater need of advice on preventing illness. With a territory-wide records system, it would be easy to track the one-time incentive. Vaccination rates would also be improved by this, reducing common diseases such as hepatitis, and the consequent treatments.
Now we move on to the discussion of financing options.
Seven financing options, but 3 basic components
In its full consultation paper, the Government proposes seven financing options, although it cunningly only attaches numbers to six of them. The unnumbered first option, which we will call "option zero" is to maintain the status quo of heavily-subsidised hospital charges, and continue exempting welfare recipients from those charges. This and the other six options are also included in a brochure summarising the proposals, but confusingly, they are renumbered 1, 2.1, 2.2, 3.1, 3.2 and 3.3, with the status quo again being unnumbered. However, it doesn't really matter, because what they all boil down to are various permutations of 3 things:
- Subsidies from government revenue
- Mandatory Insurance
- Mandatory Savings
Let's look at these three components in detail.
1. Subsidies from government revenue
Webb-site.com has always promoted free markets and civil liberties, but with a social safety net to provide a basic standard of living for those unable to pay.
There are two basic ways to provide a government subsidy for any goods or services. Price-based subsidies deliberately under-price the goods or services, while targeted subsidies provide financial support to those who cannot pay full prices, in the form of waivers or discounts. The price-based approach is politically convenient but highly wasteful, because it gives the subsidy to everyone, including those who don't need it. That approach is followed by the Government in numerous areas, including, for example, swimming pools, museums, water supply and public transport. The Hospital Authority (HA) also uses the price-based subsidy approach. About 95% of its budget comes from the Government.
The current fees and charges are just token, for example, HK$100 per night in a hospital bed, originally intended to cover basic food and beverage, $100 per attendance at an accident and emergency (A&E) unit and $100 for the first attendance at a specialist out-patient clinic. By comparison, according to the HA's latest annual report for 31-Mar-07, the HA's expenses for a visit to an A&E department were $700, and its expenses per patient per day in general acute and convalescence units were $3,290.
Even with the low fees and charges, 21% of them were waived. Waivers are provided to recipients of Comprehensive Social Security Assistance (CSSA), as well as patients whose monthly household income does not exceed 75% of the median and whose household assets do not exceed certain amounts, excluding their home if they own it. Medical Social Workers can also grant waivers on various subjective grounds such as "other justifiable social factors", all explained at this link. The maximum income and assets thresholds for HA fee waivers are higher than those to qualify for CSSA. The main intent of all this is to satisfy the principle enshrined in Section 4(d) of the Hospital Authority Ordinance that "no person should be prevented, through lack of means, from obtaining adequate medical treatment".
It is obvious that there is a lot of scope for raising fees and charges without pushing too many people into the waiver class. A night at a hospital for HK$100, including all treatment, surgery and care? You can barely go to the movies and buy a bucket of popcorn for that these days, and they don't heal you at the movies. The Government should embark on a plan to raise fees and charges (in real terms, i.e. above the rate of inflation) gradually over time, while maintaining a waiver scheme for those who cannot afford it. The increased fees could absorb a lot of the projected growth in healthcare costs, should these arise.
This increase in fees (or reduction in subsidies) with targeted waivers was in fact the recommendation of the "Scott Report" on The Delivery of Medical Services in Hospitals, commissioned by the Government in Feb-85 from W.D. Scott Pty. Co. and Coopers & Lybrand, and delivered in Dec-85. We were unable to find a copy online. It recommended increasing charges to 15-20% of actual cost. We would suggest that there is scope, at least for the initial part of each person's costs, to go further than that, and to be more creative in how the burden is spread.
Our proposal - a staggered subsidy
The flat-rate subsidy approach (where every price is discounted by the same amount) fails to recognise that most people have some financial means to handle regular fluctuations in their income and expenditure. For example, if their TV or air conditioner breaks down, they will buy a new one. Similarly, most people should be able to afford minor medical expenditure (such as casting a broken leg) at less subsidised rates, but may not be able to afford the costs of a major disease without a large subsidy. So it makes sense to adjust the subsidy accordingly.
One way to do this, rather than subsidising 80% of every charge, would be to encourage self-reliance and lower usage by charging a higher percentage of actual costs for the first dollar amount per person per year, and then to cut back thereafter. We will call this a staggered subsidy. For example, the maximum annual charge (phased in over several years) could be as follows:
| Actual cost to HA | Charge | Maximum |
|---|---|---|
| First $20,000 | 50% | $10,000 |
| Next $40,000 | 25% | $10,000 |
| Above $60,000 | 0% | Free |
We don't have enough data to accurately assess how much that would raise, and the numbers could be adjusted, but you get the overall idea. The most anyone would pay in this example would be $20,000 in one year, equivalent to about 2 months' median wage, in return for $60,000 of services. If all of that were used on in-patient treatment, taking an HA cost-per-night of $3,500, that would cover 17 nights, and the average subsidy on that would be two-thirds, with one-third paid by the patient. If you need more than 17 nights per year in hospital, then you would have nothing extra to pay.
Each citizen would know that they don't have to spend more than $20,000 in any year, but unless they are on welfare, they will have to pay up to that amount, and this gives them an incentive to take reasonable steps to stay healthy and avoid the cost. At the same time, they would know that "catastrophic" costs are effectively insured by the Government out of general revenues.
Of course, by paying out that amount, they may then end up with insufficient assets and on welfare, but that is what welfare is for - a safety net for those who have been unable or unwilling to save. Consideration could be given to exempting children under 18 and full-time students, so that parents would only have to worry about providing for their own costs.
Capping annual fees per person would of course require some form of accounting system, but as Hong Kong has a well-established ID-card system, and is proposing a system-wide electronic records system, it should not be difficult.
Accurate subsidies
We also favour more accurate subsidies. Charging a flat-rate per patient night is simple but crude, averaging all treatments across all patients. Some treatments cost much more than others, because of the drugs involved, the amount of tests, or the number of medical staff involved. With modern enterprise software, it is now easy to keep track of actual costs. Users should be presented with itemised bills showing the full cost of treatment, the amount of subsidy, and the net price. The average cost of common treatments should be published and used in educational outreach.
Fee recovery
We also see no reason to exclude a patient's self-owned home from the net assets test for determining exemption from (subsidised) fees. Clearly if all their income goes to pay the mortgage, or if the property is all they own, then they won't be able to pay much for healthcare at the point of delivery, but the HA could record long-term receivables in its accounts, accruing a market rate of interest, and when the person in question sells his property or dies, the HA should claim for the amount of (subsidised) fees still owed. Statements of amounts due should be sent annually, and those overdue by more than a year could be secured with a second mortgage on the property. Only if the deceased person's estate is insolvent should the amount be written off.
2. Mandatory insurance
The Government's proposal is that every person (possibly subject to a minimum income or assets test) would be forced to buy an insurance policy from a government-approved insurer at a standard rate, with a standard schedule of benefits. There are various ways you can do this - a population-wide scheme would charge the same premium to everyone, while it would also be feasible to divide the risk pool into age groups, so that young people pay less than older people. It is also possible to tilt the schedule of benefits towards covering the full cost of certain "lower priority" treatments which can then be out-sourced to the private sector, such as cataract operations.
Mandatory insurance means what it says - insurers would not be able to deny cover or increase your rate after you contract a long-term illness. However, the premium would have to be set annually based on the actual cost of providing healthcare to the entire population, so if healthcare costs go up as fast as the Government claims, then so will insurance premiums.
We already have a community-wide risk-sharing system - it is called the tax system. Compared with insurance, it doesn't involve any new and costly administration. Insurers would have to collect the premiums up front, then haggle with you or the hospital over whether your claims are covered, and then pay out.
The Government claims that the premiums would be set on a "no profit" basis, but in reality that would be hard to police - they probably mean no underwriting profit (premiums minus payouts and expenses), but they would allow the insurers to take the float and invest it. They would also allow the insurers to market top-up insurance for greater cover - without the insurers having to pay anything for "introducing" the clients. How they would allocate internal expenses, such as staffing, between the "no profit" and "for profit" insurance is open to manipulation.
There is a risk that over time, the Government would raise the level of co-payments that the patient would have to pay towards each treatment under the basic plan, or limit the annual claims per person under the basic plan, thereby pushing the public into buying top-up insurance. Unlike the basic plan, top-up insurance would be for-profit, and coverage could be denied to the higher risk patients or for pre-existing illness, or their premiums raised to cover it. You see, insurance only works if there is uncertainty about the outcome. If you are known to have cancer, and certain to require more treatment next year, then any insurer would have to charge you to cover the cost, and the insurance would be pointless.
Mandatory insurance also runs the risk of cost escalation through excessive billing by private clinics or unnecessary tests or drugs, whereas a user-pays subsidised system, in a public health system with no profit motive, can deter this.
Mandatory insurance would also shift the burden of coverage towards the lower and middle income groups, because everyone would pay the same rate, whereas in a tax-based system the higher incomes subsidise those on middle and lower incomes.
3. Mandatory savings
Little needs to be said about this. Forced savings, like forced insurance, are an intervention in personal choice. Savings do not spread risk, and anyone with a serious illness in the family would quickly blow through their mandatory savings and have to fall back on their other savings or seek waivers of medical fees in the social safety net. Experience of the MPF has shown that forced savings, where money is handed over to banks and institutions, is very costly to operate, clocking up administration and management fees of over 2% per year on funds under management, which eats away 45% of the capital and returns over a 30-year period. The MPF was a big enough gift to the fund management industry, and we see no reason to give it another one - we continue to call for abolishing or reforming the MPF.
The politics
In our view, the mandatory insurance and mandatory savings aspects of these proposals are partly a payback for political support of the insurance and finance sectors in the electoral system for the Chief Executive. The proposals would also satisfy those tycoons who believe, wrongly in our view, that if Hong Kong becomes a democracy rather than a plutocracy, then it will automatically become a high-tax welfare state and bleed employers dry, unless schemes like this are installed to prevent it, before we have democracy.
The schemes would involve vast amounts of administration costs, as the MPF has demonstrated. As for insurance, by the Government's own admission, at least 5%, probably more, of the insurance premiums would go in administration costs, while as noted above, the Government may pitch the basic insurance at an insufficient level of coverage of increased HA charges, particularly for major illnesses where limits are hit, and then allow insurers to profit from selling top-up insurance on the back of the mandatory insurance.
For readers outside Hong Kong, it is helpful to explain some of the influences on the proposals. The tycoon-funded Bauhinia Foundation (BF) on 24-Aug-07 published a report titled "Development and Financing of Hong Kong's Future Health Care". This followed a preliminary report on 10-Jul-07, just 10 days into Donald Tsang's second term as Chief Executive. Three of the four directors of BF are government-appointed members of the Hospital Authority, including the Chairman of both, and our article today "Who is the Bauhinia Foundation?" examines the connections and secretive funding of the BF.
In the BF report, they proposed in essence a freezing of the current level of services in the HA (what they called "Pillar 1"). New technologies, advanced surgery procedures, shorter waiting times for non-urgent conditions, health screening and early detection services would be provided in "Pillar 2", which would be 50% subsidised if you were in a mandatory savings account (MSA), funded by employee contributions, which they proposed be collected through the existing MPF system. Employer contributions would be "voluntary". Low income groups would not have access to these new "Pillar 2" services, because they would not contribute to MSAs. People would be allowed to draw from their MSA to buy approved medical insurance in the private sector. There was also a proposed "Pillar 3" consisting of unsubsidised private healthcare, but we already have that in the market.
Tax treatment
Currently, if an employer provides medical insurance to an employee, then the employer deducts the expense from taxable income, while the employee does not get taxed on the benefit, as it cannot be converted into cash. But if an employee buys his own medical insurance, then he has to do so out of his taxed income. This is unfair. To remove the inequity and encourage voluntary medical insurance, people who buy their own insurance should get a deduction of the cost against their income for salaries tax purposes.
Vehicle and workplace accidents
There are some types of healthcare, such as treating injuries from vehicle accidents and workplace injuries, where the full cost should be covered by insurance. Currently all vehicle drivers are required to be insured for third party liability, and all employers are required to carry employee compensation insurance up to HK$100m for one event, so it is reasonable then to recover the full cost of this healthcare and not to burden the public finances with it.
To avoid false claims, public hospitals should charge the patient on the usual subsidised basis, and the patient can then recover his payment from the insurers. Meanwhile, the hospital should have a right of action (with statutory backing if necessary) to recover the subsidy from the insurers involved. The mandatory vehicle insurance should be extended to include not just third party injuries (including passengers) but the driver himself, and the liability for injuries should be divided equally amongst the insured vehicles involved, so that if, for example, there are 2 vehicles in a collision, then the insurer of each picks up half the healthcare costs without arguing about whose fault it was. Put that in law and the vehicle insurance premiums will adjust accordingly.
No sugar
In an unsubtle attempt to sweeten the bitter pill of forced savings, the Government has suggested that $50bn of our $1104bn of reserves should be injected into medical savings accounts at the start, or about HK$7,100 per person. This is already public money, and could just as easily be used to subsidise an improved healthcare system directly. You can be confident that it would not be possible to withdraw this money from your Mandatory Savings Account and walk off with it, so don't be fooled into regarding this as a hand-out.
So in summary, we propose:
- A staggered subsidy, replacing the current flat-rate subsidy, so that a higher portion, say 50%, of the first part of each person's annual costs is paid by them.
- A cap on the annual fees chargeable to each person, at say HK$20,000, so that anything above that is covered by the state, in effect providing state-insured catastrophe risk.
- A phased reduction of overall subsidy from 95% to 80%, say over 5 years.
- Continued exemption for those on welfare, but refining the means test to make sure that those who can pay the subsidized fees do, if necessary by deferring the fees until they sell their property or die.
- No mandatory insurance or savings.
- Salaries tax deduction for voluntary health care insurance purchased by employees (employers already get this deduction from taxable profits).
- Creative schemes to incentivise screening, early detection and education, such as offering to pay people to be tested for major risks, if it will reduce treatment expenditure in the long run.
- The Hospital Authority to recover from insurers the full costs of subsidies for treating vehicle and workplace accident victims.
What do you think? Take our Healthcare poll
© Webb-site.com, 2008
Topics in this story
Sign up for our free newsletter
Recommend Webb-site to a friend
Copyright & disclaimer, Privacy policy


